|
1/18/2024 0 Comments Gilead coupon truvada 
A 30-day supply of PrEP (brand-name Truvada) can cost nearly $2,000. The biggest impact for the community their organizations serve may be for PrEP - a daily pill that helps prevent HIV infection, says Carl Schmid, deputy executive director at the AIDS Institute, an advocacy group. Shots - Health News PrEP Campaign Aims To Block HIV Infection And Save Lives In D.C. Among the top 200 drugs (based on spending) in 2014, the study found that 132 were brand-name drugs, and 90 of them offered copay coupons. In 2016, 20 percent of prescriptions for brand-name drugs used a drug copay assistance coupon, according to an analysis by researchers at the USC Schaeffer Center for Health Policy and Economics. But, he argues, assistance programs for drugs that are available from more than one source - such as a brand drug that is also available as a generic - shouldn't be allowed. Marcotte says that if there is no other comparable drug available, drug copayment programs may have a role to play if they can be structured so that participating patients are paying some amount toward their deductible. Fifty-six percent say they're considering them for 2019 or 2020. In an NBGH survey of about 140 multistate employers with at least 5,000 workers, 17 percent report they have a copay accumulator program in place this year, Marcotte says. If someone needs medical care such as surgery, for example, that person doesn't get help covering his deductible, he says. "From an employer perspective, everyone under the plan has to be treated the same," says Brian Marcotte, president and CEO of the National Business Group on Health, which represents large employers. 
There's also the issue of fairness, they say. Some employers argue that the drug copayment programs are an attempt to circumvent their efforts to manage health care costs. Most annual copay assistance limits for MS drugs, if available, are between $9,000 and $12,000, Talente says. "Most have different mechanisms of action, different administration and different side effect profiles." And generics, when they're available, are pricey too - typically costing $60,000 or more annually, she says. "Generally the multiple sclerosis drugs are not substitutable," she says. 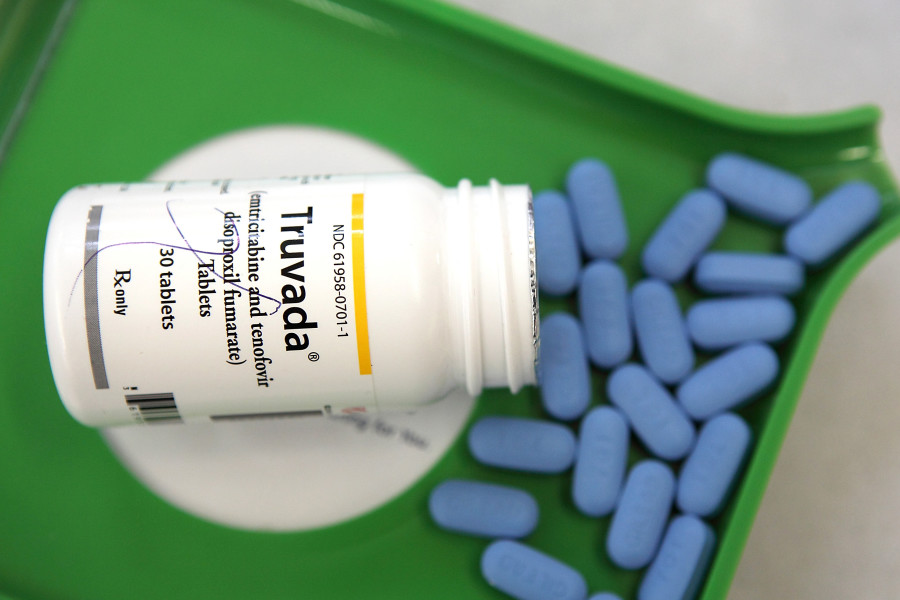
That last argument misses an important point, according to Bari Talente, executive vice president for advocacy at the National Multiple Sclerosis Society. But, she says, her family can't afford to pay nearly $9,000 a year out-of-pocket for the foreseeable future. In Catton's case the change meant that after she hit the drug manufacturer's payment cap for the copay assistance in April, she's had to pay the entire co-payment herself - roughly $3,800 - and will have to continue to pay it until her health plan's pharmacy deductible is met.įor May, Catton has put the $3,800 copay on a credit card. Under the copay accumulator programs introduced by some health plans in 2018, the process has changed. Through such programs, consumers typically have owed nothing or have had modest monthly copays for pricey drugs, thanks to a financial contribution by the drugmaker that chips away at the consumer's deductible and out-of-pocket maximum limits until the health plan starts paying the whole tab. Her health plan changed the way it handles Novartis' payments, and the money no longer counts toward that deductible.Ĭatton is one of a growing number of consumers taking expensive medicine who are discovering they are no longer insulated by copay assistance programs that used to help cover their costs. The drug's price: $90,000 each year.īut his year, Catton got a shock. Hospital nurse Kristen Catton relies on medication to keep her multiple sclerosis in check. Until recently those payments by the drug company helped Catton save money on her medical out-of-pocket expenses, because they counted toward her family's $8,800 annual pharmacy deductible on their health plan. Novartis, the company that makes Gilenya, helps defray that cost for Catton and other patients by making their copayments directly to the patient's health plan Catton's copay for the medicine is roughly $3,800 a month. The drug is expensive - about $90,000 a year. This is a big step forward two drugs she previously tried failed to control her physical symptoms or prevent repeated flare-ups. Thanks to the medicine, she says, she's able to walk comfortably, see clearly and work part time as a nurse case manager at a hospital near her home in Columbus, Ohio. Since Kristen Catton started taking the drug Gilenya two years ago, she's had only one minor relapse of her multiple sclerosis, following a bout of the flu. As the price of specialty drugs continues to rise, some health plans are shifting more of the cost to patients. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
